When you hear “heel pain,” most people immediately think of plantar fasciitis. While plantar fasciitis is the most common cause, there are several other conditions that can mimic its symptoms, and getting the diagnosis right is crucial for effective treatment.
Today, I’ll take you through four conditions that cause heel pain but aren’t plantar fasciitis, how to spot the differences, and why seeing a podiatrist matters.
Achilles Tendinopathy
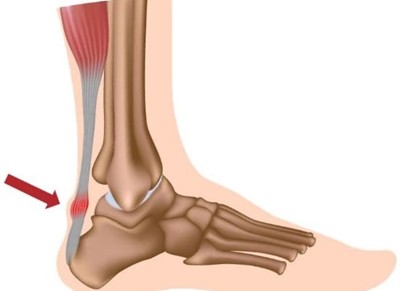
What it is: Achilles tendinopathy is a condition where the Achilles tendon, which connects your calf muscles to your heel bone, becomes irritated or degenerated.
How it presents:
- Pain and stiffness at the back of the heel or just above it.
- Swelling or thickening along the tendon.
- Pain that worsens with activity, especially running, jumping, or uphill walking.
- Morning stiffness that improves slightly with movement.
How it’s different from plantar fasciitis:
- Location: Achilles pain is behind the heel; plantar fasciitis pain is usually under the heel and often closer to the arch.
- Type of pain: Achilles tendinopathy feels more like an aching or pulling sensation, while plantar fasciitis often feels sharp or stabbing when first standing after rest.
- Activity pattern: Achilles tendinopathy pain tends to build during activity, while plantar fasciitis often flares after rest or first thing in the morning.
Treatment differences:
- Achilles tendinopathy requires a focus on gradual loading exercises to strengthen the tendon.
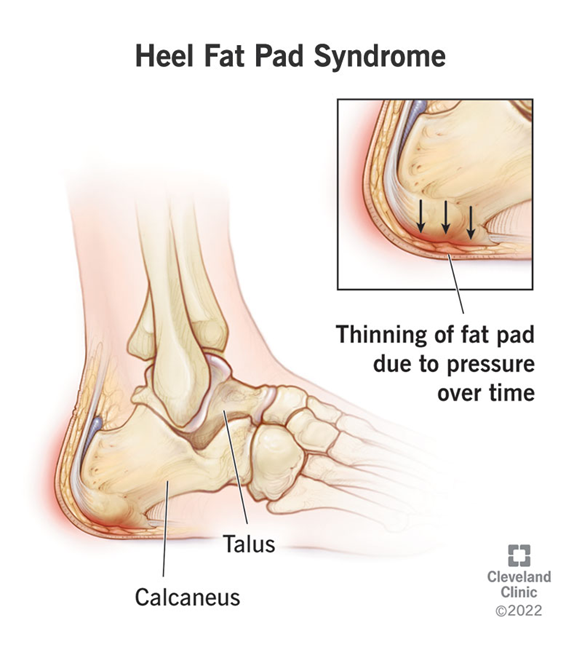
Heel Fat Pad Atrophy
What it is: The heel fat pad is a thick cushion of fatty tissue that protects your heel bone when you walk. Over time, this pad can thin out (atrophy) or become damaged, leading to a lack of natural cushioning.
How it presents:
- A deep, bruised feeling in the middle of the heel.
- Pain worsens when walking on hard surfaces or barefoot.
- Less “sharp” pain – more of a dull, achy, bruised sensation.
How it’s different from plantar fasciitis:
- Location: Heel fat pad pain is felt centrally under the heel, while plantar fasciitis pain is often more towards the front of the heel near the arch.
- Pain triggers: Fat pad atrophy pain is worse with direct pressure, while plantar fasciitis is worse with first steps after rest.
- Physical signs: Thinning or flattening of the heel pad can often be seen or felt.
Treatment differences:
- Fat pad issues require cushioning, not stretching. Soft heel cups and supportive footwear with a thick outer sole are essential.
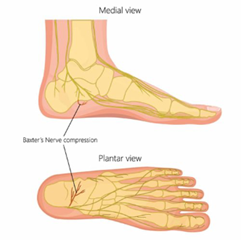
Baxter's Nerve Entrapment
What it is: Baxter’s nerve is a small branch of the lateral plantar nerve that runs along the inside of the heel. It can become compressed, causing nerve pain.
How it presents:
- Sharp, burning, tingling, or shooting pain under the heel or into the arch.
- Symptoms may worsen with standing for long periods or particular foot movements.
- Slight numbness or pins-and-needles sensation.
How it’s different from plantar fasciitis:
- Neurological symptoms: Tingling, burning, or numbness usually indicates nerve involvement, which is not typical in plantar fasciitis.
- Pain character: Nerve pain tends to be more “electric” or burning, whereas plantar fasciitis is usually a ”sharp,” stabbing pain when weight-bearing after rest.
- Clinical tests: To test for Baxter’s nerve entrapment, your podiatrist will tap along the path of the nerve. If this elicits a tingling sensation, the test is considered positive for nerve compression.
Treatment:
- Management of Baxter’s nerve entrapment involves offloading nerve pressure (e.g. with appropriate footwear and orthotics where required), exercises, and sometimes additional treatments like dry needling, shockwave or laser.
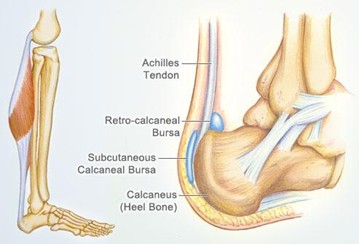
Heel Bursitis
What it is: Bursae are small fluid-filled sacs that cushion and reduce friction between tissues. In the heel, bursitis can occur in several areas:
- Retrocalcaneal bursitis – between the Achilles tendon and heel bone.
- Subcutaneous calcaneal bursitis – between the skin and the heel bone, often due to shoe pressure.
- Sub-calcaneal plantar bursitis – under the heel, between the plantar fascia and heel bone.
How it presents:
- Swelling, tenderness, and warmth over the affected area.
- Pain when pressing directly on the bursa location.
- Pain worsened by certain shoes – patients often feels better barefoot for subcutaneous calcaneal bursitis
- In retrocalcaneal bursitis, pain may increase with ankle motion, particularly pointing the toes.
How it’s different from plantar fasciitis:
- Location-specific swelling: Bursitis often causes visible or palpable swelling, which is not typical with plantar fasciitis.
- Pain on compression: Applying pressure to the specific bursa area often reproduces the pain.
- Pain with footwear: Subcutaneous bursitis pain often worsens from direct shoe contact, while plantar fasciitis pain is usually related to movement.
Treatment differences:
- Treatment focuses on reducing inflammation and offloading pressure. This may include footwear changes (padding to offload the bursa within the shoes), heel lifts, NSAIDs, and laser therapy to settle inflammation.
Why It’s So Important to See a Podiatrist
Many heel pain conditions can seem similar at first, but the differences in location, pain type, and what triggers the symptoms are vital to getting an accurate diagnosis. Treating the wrong condition can delay healing and even make things worse.
At Galleria Podiatry Perth, we perform thorough biomechanical assessments to determine the exact cause of your heel pain and create a personalised treatment plan that gets you back on your feet.
Don’t put up with heel pain – book an appointment today and take the first step toward recovery!
Ready to give your feet the care they deserve? Book an appointment with one of our podiatrists in Perth.

